Sphenopalatine ganglion (SPG) block has been used for the treatment of headaches and other pain conditions for over 100 years. The original method involved placing a long Q-tip-like cotton swab dipped in cocaine through the nose and against the SPG.
SPG is the largest collection of nerve cells outside the brain and it sits in a bony cavity behind the nasal passages. These nerve cells are closely associated with the trigeminal nerve and include sensory nerves, which supply feeling to parts of the head and autonomic nerves, which regulate the function of internal organs, blood vessels, as well as tearing and nasal congestion. Considering that these nerve cells produce such a wide range of effects, it is logical to expect that blocking these nerves might help headaches.
For obvious reasons we no longer apply cocaine, but instead use numbing medicines, such as lidocaine or bupivacaine. A small study suggested that just putting lidocaine drops into the nose can relieve an acute migraine. I’ve prescribed lidocaine drops to some patients with cluster headaches and a small number reported relief. The problem with nasal drops is that we are not sure if lidocaine actually reaches all the way back to numb the SPG even if they are lying down with the head hanging back over the edge of the bed. Using long Q-tips is uncomfortable and in many patients the Q-tip may also not reach the SPG.
To solve the problem, two doctors developed thin intranasal catheters that appear to consistently reach the area of SPG. Dr. Tian Xia’s Tx360 device seems to be more comfortable for patients because his is a thinner and a more flexible catheter. The recommended local anesthetic is bupivacaine (Marcaine), which lasts longer than lidocaine. A small double-blind study of SPG block using Tx360 in chronic migraine patients showed it to be effective. The active group had a reduction of the Headache Impact Test (HIT-6) score, while the placebo group did not. In this study patients were given the SPG block twice a week for 6 weeks. We need larger and longer-term studies in chronic migraine patients before advising such frequent regimen, not in the least because of cost.
SPG block seems to be more appropriate (and this is what we use it for at the NYHC) for patients with an acute migraine that does not respond to oral or injected medications and for those with cluster headaches. Since cluster headaches usually last for a few weeks to a couple of months (unless it is a patient with chronic cluster headaches), it is practical to try SPG blocks on a weekly basis. Theoretically, because there is so much autonomic nervous system involvement in cluster headaches (tearing, nasal congestion, and other), SPG should be particularly effective for cluster headaches.
Another way to affect the SPG is by stimulating it with electrical current, which seems to be effective for chronic cluster headache patients, according to a small study. This method requires surgical implantation of a device into the area of the SPG. See my previous post on this.
Below is an illustration of the SPG and the Tx360 device.
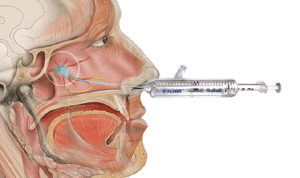
.png)


